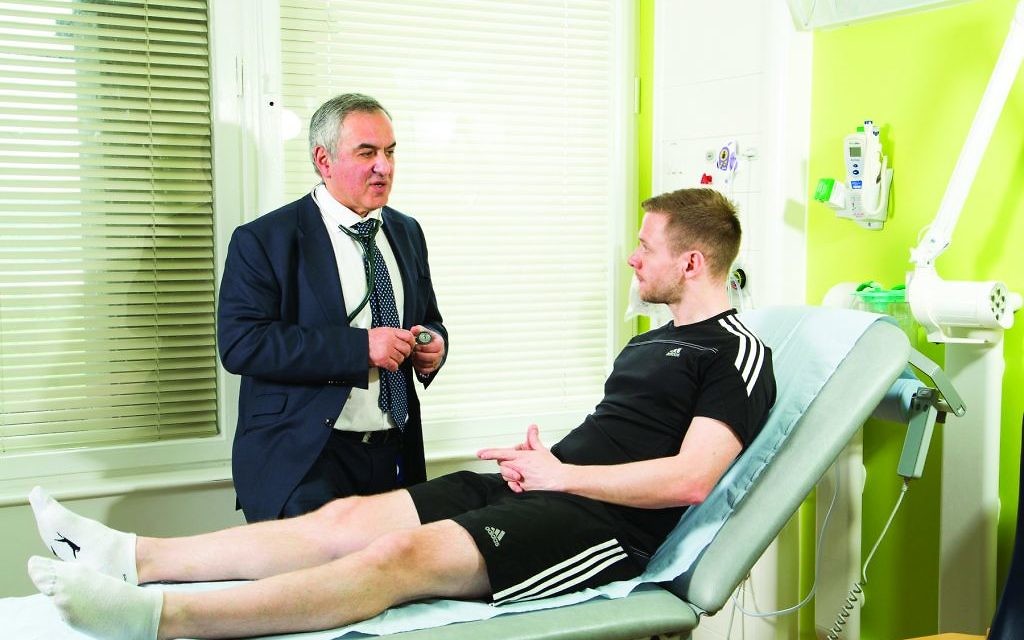
Putting patients at the heart of care
Dr Joseph Davar, consultant cardiologist at the Royal Free Hospital, talks to Deborah Cicurel about his rewarding career
As a challenging and prestigious career, being a cardiologist no doubt has its trials – but as one leading doctor has shown, the job has its many rewards too.
Dr Joseph Davar, a consultant cardiologist at the Royal Free Hospital, and an honorary senior lecturer at UCL, has worked as a cardiologist for more than 30 years, travelling everywhere from Georgia to Russia as part of his studies and publishing papers, chairing committees and supervising research projects in the process.
But Dr Davar had not always dreamed of being a cardiologist: it was in his third year of medical school that he knew what he wanted to.
“The cardiovascular unit of a student research facility was one of the first to be opened and I started to participate in experiments,” he explains. “In the fifth year, I became the head of a student research team studying the effects of different types of surgery on the heart.
“But my ‘eureka’ moment came when I saw the living, beating heart of a patient on the screen of an ultrasound machine.
“I was fascinated by the ability to look into the heart and assess what was wrong without causing any harm to the patient. It was at this time that my lifelong affair with cardiology and imaging started.”

Dr Davar has seen a great range of heart problems, but the advice he gives to young people to help them prevent future issues has been consistent. “Cultivate healthy habits, as habits tend to persevere throughout life. Enjoy regular physical activity and enjoy the taste of water rather than sugary drinks,” he says. “Realise that a diet full of vegetables and fruit – but more vegetables – is healthier, and far more nutritious than high fat and sugary snacks. Avoid smoking and watch your alcohol consumption. Try to reduce the time spent at the computer, tablet and in front of the television – it’s much more interesting to live than to watch how others do it.”
I ask Dr Davar whether heart problems are predetermined – are they preventable or mostly genetic? The answer is both.
“Many health problems, including cardiological ones, are due to a combination of genetic and environmental factors,” he says.
“Controlling or modifying certain environmental factors, especially from a young age, by diet and physical activity could definitely contribute to avoid or lessen the impact of the genetic database we are born with.”
And what of the stresses of modern life? Surely our fast-paced lifestyles, crazed schedules and inability to switch off are factors in causing heart problems?
“There are many factors contributing to the high prevalence of hypertension and stress is one of them,” Dr Davar says.
“The perception of a hectic lifestyle, or an almost constant lack of time, leads to certain traits such as sleep deprivation, unhealthy diets high in salt, sugar and processed food and low levels of physical activity. Subsequently, there’s a higher prevalence of people with a raised body mass index, especially those with a high waist circumference, diabetes and so on, all contributing to the development of hypertension.”
It’s not all bad news. We can prevent development or reverse some of the effects of high blood pressure and heart problems if we modify our lifestyles, according to the doctor. “The main issue to highlight is that it is possible to change aspects of one’s life to try to prevent the development of hypertension.”
“What is important is to realise that by walking a reasonable amount every day, paying attention to our weight, salt, sugar and overall calorie intake, we can reduce significantly the chance of developing many cardiac problems.”
So is the Jewish community at any greater risk of developing heart issues than the rest of the population? “There are certain types of genetically-determined conditions somewhat more prevalent in selected groups of the Jewish population and could involve the heart,” Dr Davar says. “Plus, traditional Jewish cuisine can be quite fatty, sugary and salty. My grandmother cooked a delicious chicken soup, but also used chicken fat to roast and fry potatoes.”
However, despite what our Shabbat dinner tables may look like, Dr Davar believes the community is healthier than ever. “Overall, the Jewish population has become well aware of the benefits of a healthy and balanced diet,” he says.
While Dr Davar faces daily challenges in his work, it has its rewards – especially when he knows how medicine has helped to transform lives. “To see a patient who had a serious and complicated course of illness walking along the street and smiling is most rewarding,” he adds.
Contact Dr Davar, MD PHD, FRCP, FACC, via the Royal Free London Private Patients Unit, 020 7317 7751, rf.privateenquiries@nhs.net, or visit royalfreeprivatepatients.com

Thank you for helping to make Jewish News the leading source of news and opinion for the UK Jewish community. Today we're asking for your invaluable help to continue putting our community first in everything we do.
For as little as £5 a month you can help sustain the vital work we do in celebrating and standing up for Jewish life in Britain.
Jewish News holds our community together and keeps us connected. Like a synagogue, it’s where people turn to feel part of something bigger. It also proudly shows the rest of Britain the vibrancy and rich culture of modern Jewish life.
You can make a quick and easy one-off or monthly contribution of £5, £10, £20 or any other sum you’re comfortable with.
100% of your donation will help us continue celebrating our community, in all its dynamic diversity...
Engaging
Being a community platform means so much more than producing a newspaper and website. One of our proudest roles is media partnering with our invaluable charities to amplify the outstanding work they do to help us all.
Celebrating
There’s no shortage of oys in the world but Jewish News takes every opportunity to celebrate the joys too, through projects like Night of Heroes, 40 Under 40 and other compelling countdowns that make the community kvell with pride.
Pioneering
In the first collaboration between media outlets from different faiths, Jewish News worked with British Muslim TV and Church Times to produce a list of young activists leading the way on interfaith understanding.
Campaigning
Royal Mail issued a stamp honouring Holocaust hero Sir Nicholas Winton after a Jewish News campaign attracted more than 100,000 backers. Jewish Newsalso produces special editions of the paper highlighting pressing issues including mental health and Holocaust remembrance.
Easy access
In an age when news is readily accessible, Jewish News provides high-quality content free online and offline, removing any financial barriers to connecting people.
Voice of our community to wider society
The Jewish News team regularly appears on TV, radio and on the pages of the national press to comment on stories about the Jewish community. Easy access to the paper on the streets of London also means Jewish News provides an invaluable window into the community for the country at large.
We hope you agree all this is worth preserving.
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)