Ashkenazi cancer study leads to calls for overhaul of screening process
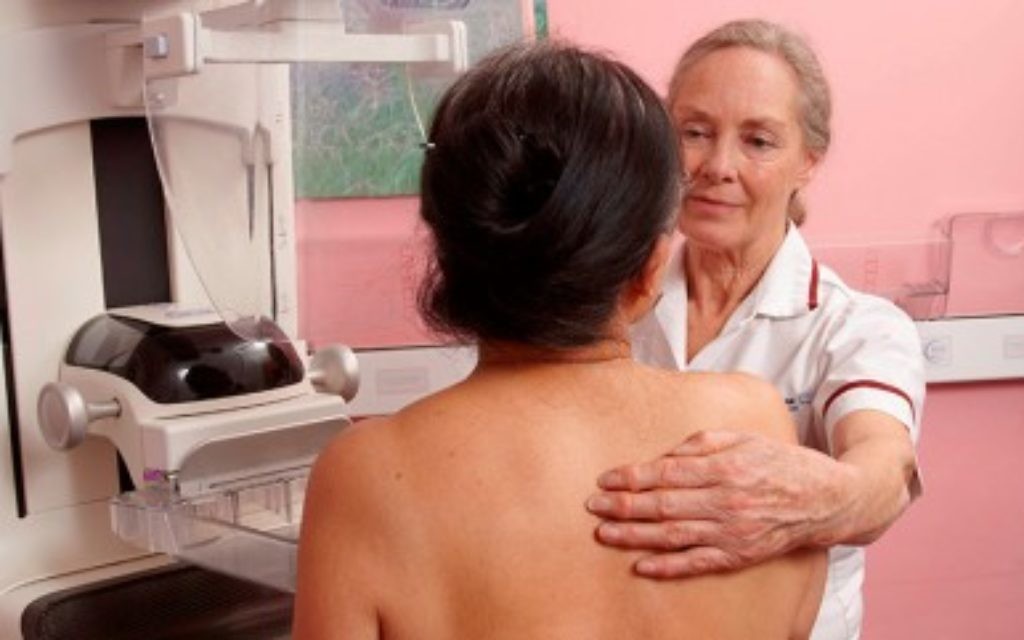
 A huge study into testing for cancers in the Ashkenazi Jewish community has led to calls for the screening process to be overhauled.
A huge study into testing for cancers in the Ashkenazi Jewish community has led to calls for the screening process to be overhauled.
Researchers say the work shows that by offering testing to the whole population of Ashkenazi Jews it would detect 56% more people with cancer-related BRCA mutations, compared to the current way of testing which is based on family history.
The study by the Genetic Cancer Prediction through Population Screening Study (GCaPPS), funded by the Eve Appeal, allays concerns that such ‘population screening’ would affect adversely affect Jewish women’s quality of life or psychological state.
Get The Jewish News Daily Edition by email and never miss our top stories Free Sign Up
It also shows that by offering screening to all Ashkenazi Jewish women aged 30+ for BRCA mutations, it would save the NHS money, when health bosses had asked whether such a roll-out would be cost effective.
Those with Ashkenazi Jewish descent have a much higher prevalence of harmful BRCA1 and BRCA2 mutations than the rest of the population, with one in 40 known to be carriers, compared to a national average of one in 800 women.
Women carrying these altered genes have a 45% to 65%% chance of getting breast cancer in their lifetime, and a 15% to 45% chance of getting ovarian cancer. Treatment can mean having the ovaries, fallopian tubes and/or breasts removed.
But current NHS testing is only offered to people on the basis of well-defined criteria, involving a personal or family history of breast and ovarian cancer.
However the authors argue in the Journal of the National Cancer Institute this week that screening the whole Ashkenazi Jewish population “would reduce the number of ovarian and breast cancers and save the NHS £3.7 million”.
Using economic models, they show that if 71% of the eligible 114,000 women are screened, this would mean 276 less ovarian cancers and 508 fewer breast cancers.
“The study provides valuable evidence for reviewing the national screening process for cancers within specific populations,” said a spokeswoman for the Eve Appeal.
Significant findings for #Ashkenazi #Jewish women in new study from @TheEveAppeal & @uclnews published in @JCNI_Now today @BBCHughPym
— The Eve Appeal (@TheEveAppeal) December 1, 2014
Thank you to @BootsOfficialUK for supporting our research study on #cancer risks #Ashkenazi #Jewish women published in @JCNI_Now today
— The Eve Appeal (@TheEveAppeal) December 1, 2014

Thank you for helping to make Jewish News the leading source of news and opinion for the UK Jewish community. Today we're asking for your invaluable help to continue putting our community first in everything we do.
For as little as £5 a month you can help sustain the vital work we do in celebrating and standing up for Jewish life in Britain.
Jewish News holds our community together and keeps us connected. Like a synagogue, it’s where people turn to feel part of something bigger. It also proudly shows the rest of Britain the vibrancy and rich culture of modern Jewish life.
You can make a quick and easy one-off or monthly contribution of £5, £10, £20 or any other sum you’re comfortable with.
100% of your donation will help us continue celebrating our community, in all its dynamic diversity...
Engaging
Being a community platform means so much more than producing a newspaper and website. One of our proudest roles is media partnering with our invaluable charities to amplify the outstanding work they do to help us all.
Celebrating
There’s no shortage of oys in the world but Jewish News takes every opportunity to celebrate the joys too, through projects like Night of Heroes, 40 Under 40 and other compelling countdowns that make the community kvell with pride.
Pioneering
In the first collaboration between media outlets from different faiths, Jewish News worked with British Muslim TV and Church Times to produce a list of young activists leading the way on interfaith understanding.
Campaigning
Royal Mail issued a stamp honouring Holocaust hero Sir Nicholas Winton after a Jewish News campaign attracted more than 100,000 backers. Jewish Newsalso produces special editions of the paper highlighting pressing issues including mental health and Holocaust remembrance.
Easy access
In an age when news is readily accessible, Jewish News provides high-quality content free online and offline, removing any financial barriers to connecting people.
Voice of our community to wider society
The Jewish News team regularly appears on TV, radio and on the pages of the national press to comment on stories about the Jewish community. Easy access to the paper on the streets of London also means Jewish News provides an invaluable window into the community for the country at large.
We hope you agree all this is worth preserving.
-
By Brigit Grant
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)
-
By Laurent Vaughan - Senior Associate (Bishop & Sewell Solicitors)